Dr. Batul Patel (Dermatologist)
Medical Director – The Bombay Skin Clinic
Dr. Batul Patel is an award winning certified dermatologist, honoured as the “Dermatologist of the Year 2023” at the national level by The Economic Times. View profile
What Is Eczema | Eczema Symptoms | Eczema Treatment Options | Safety & Results Timeline | Price
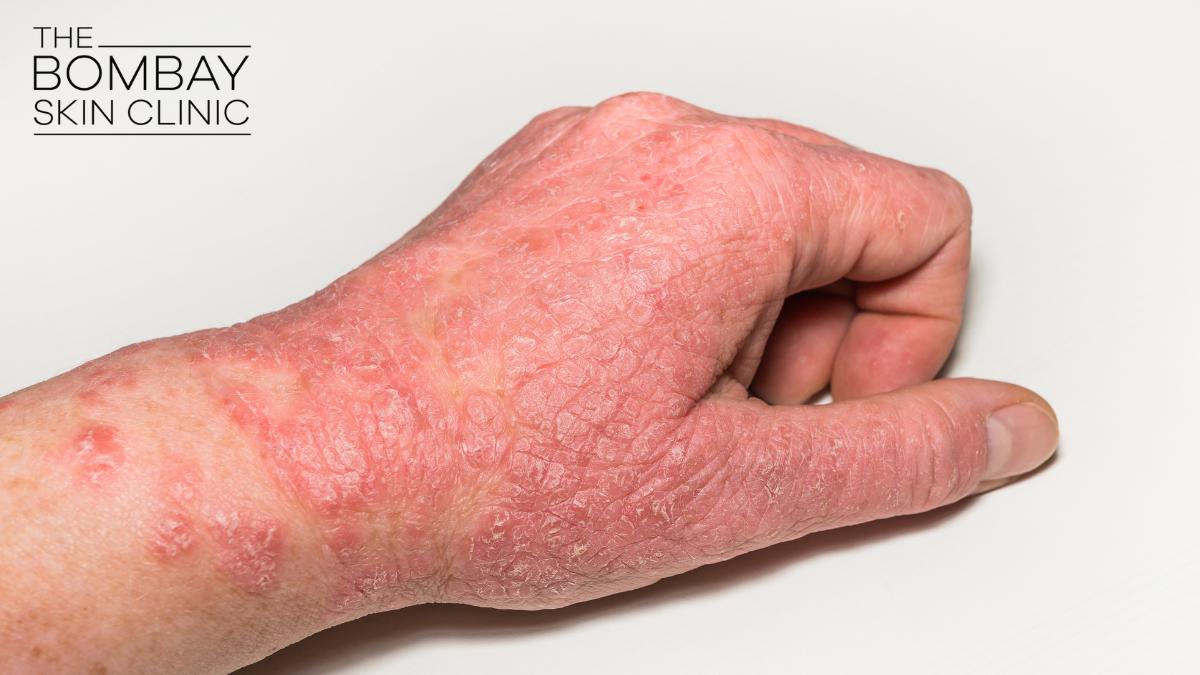
Eczema, also called atopic dermatitis, is a common long-term skin condition where the skin becomes dry, red and very itchy. It can affect babies, children and adults and often flares up from time to time.[1–4]
For many people in Mumbai, eczema is not just a skin problem. It can disturb sleep, affect work or studies, and make day-to-day life feel difficult. The good news is that with the right diagnosis, regular skincare and evidence-based medical treatment, most people can get good control over flares and feel more comfortable in their own skin.[1–4]
What is eczema (atopic dermatitis)?
What happens to the skin in eczema?
In eczema, the outer layer of the skin (skin barrier) does not work as well as it should. The skin loses more water, becomes dry and lets in irritants, allergens and microbes more easily.[1,3,5] This leads to:
- Dry, rough or scaly patches
- Redness or darkening of the skin, depending on your natural skin tone
- Intense itching, especially at night
- Cracks, oozing or crusting when the skin is very inflamed
Eczema is influenced by both genes and environment. Many people with eczema or their family members also have asthma, allergic rhinitis or other allergies.[3,6]
Is eczema the same as “skin allergy”?
Many people in Mumbai use the words eczema, dermatitis and skin allergy interchangeably. They are related but not exactly the same.
- Eczema or atopic dermatitis is a specific chronic inflammatory skin disease with typical patterns and age-wise distribution.[1,3]
- Skin allergy is a broader term and may include contact dermatitis (reaction to metal, fragrances, hair dye etc.), drug allergy and more.[4,7]
Your dermatologist will examine the pattern, location and history of your rash and, where needed, do tests to confirm the exact type.
Types of eczema we commonly see in Mumbai
Atopic dermatitis
This is the classic type of eczema. It often starts in childhood but can appear at any age. In babies it usually affects the cheeks and outer limbs. In older children and adults it more often involves the neck, eyelids, inner elbows, back of knees and hands.[3,6]
Hand eczema
Hand eczema is very common in Mumbai, especially after frequent hand washing, cleaning activities, food handling or use of harsh sanitisers. The skin on the hands becomes dry, cracked and itchy, sometimes with painful fissures.[3,7]
Nummular / discoid eczema
In this type, coin-shaped itchy patches appear on the arms, legs or trunk. They can ooze or crust during flares. It often needs careful moisturising and topical medicines to calm down.[4,5]
Seborrhoeic eczema and other mixed patterns
Some people have eczema-like patches on oily areas such as the scalp, sides of nose, eyebrows and chest, often called seborrhoeic eczema. Others may have overlapping features of different eczema types. A dermatologist’s eye helps separate these conditions and decide the best approach.
Signs, symptoms and when to see a dermatologist
Early warning signs you should not ignore
You should consider a dermatologist review if you notice:
- Dry, itchy skin lasting more than two weeks
- Repeated “rashes” in the same areas, especially bends of elbows, behind knees, neck and eyelids
- Thickened, rough or darkened skin from constant scratching
- Sleep disturbance due to itching
- Regular need for over-the-counter creams without long-term relief
Red-flag symptoms that need urgent medical help
Do not wait for your routine appointment if you develop:
- Sudden spreading redness, warmth, pus, yellow crusting or painful skin (possible infection)[1,4]
- Fever, feeling unwell along with a flare
- Eye redness, eye pain or vision changes when eczema is around the eyes
- Widespread fluid-filled blisters or erosions
These can sometimes indicate a serious infection or complication and should be assessed quickly in clinic or emergency care.
Advantages of dermatologist-led eczema treatment
Medical diagnosis instead of “trial and error” creams
Many patients reach us after months of using strong over-the-counter steroid mixes or fairness creams. Dermatologist-led care focuses first on an accurate diagnosis and classifying the severity. This reduces confusion, unnecessary products and delays in getting relief.[1–4]
Barrier repair and long-term skin health
Good eczema care is not only about calming today’s flare. We focus on rebuilding the skin barrier with moisturisers, gentle cleansers and trigger control so your skin stays more stable in the long term.[1,3,5]
Reduced flares and better sleep / daily comfort
With a structured plan, many people see fewer and less intense flares over time. Itching often reduces, sleep improves and it becomes easier to manage office work, school and social life.[1,6]
Fewer scars, marks and infections
Timely treatment helps lower the risk of skin infections, continuous scratching and post-inflammatory pigmentation (dark marks). This is particularly important in Indian skin tones, where marks can linger if flares are not controlled properly.[3,7]
Personalised plan for Mumbai’s weather and lifestyle
Mumbai’s humid, hot, coastal environment, frequent air conditioning and daily travel all affect eczema. We customise moisturising routines, bathing advice and product choices according to your lifestyle and the area of the city you live or work in.
Who is eczema treatment suitable for?
Who usually benefits from clinic-based eczema care
Eczema management at The Bombay Skin Clinic can be helpful for:
- Babies, children and adults with dry, itchy, recurring rashes
- People whose “sensitive skin” is not improving with home care alone
- Patients who have tried many creams without proper guidance
- Those with disturbed sleep, work productivity or self-confidence due to eczema
When treatment needs extra caution or specialist referral
Certain situations need more careful planning and sometimes joint care with other specialists:
- Severe, widespread eczema covering large body areas
- Eczema with asthma, food allergy or allergic rhinitis needing allergy input[3,6]
- Suspected contact allergy to metals, cosmetics, hair colour or occupational exposures
- Very frequent skin infections or poor response to standard treatment
Who may not be suitable for certain medicines or procedures
Some treatment options may not be suitable or may need modification in people with:
- Pregnancy or breastfeeding
- Uncontrolled diabetes, high blood pressure or other chronic illnesses
- Active infections, liver or kidney disease
- History of certain immune system or blood disorders
In these cases, your dermatologist will discuss safer alternatives, regular monitoring and whether to involve your physician in shared care.[1–4]
How we diagnose eczema at The Bombay Skin Clinic
Medical history and trigger mapping
We start by taking a detailed history. This includes:
- Age at which the rash started and how it has changed over time
- Family history of eczema, asthma or allergies[3,6]
- Work profile, hobbies and daily exposures (soaps, detergents, cosmetics, hair colour, metals etc.)
- Seasonal changes, stress and food history as relevant
- Previous treatments used and response
Skin examination
Your dermatologist examines the skin closely to see:
- Exact areas involved and pattern (flexural, facial, hand, nummular etc.)
- Degree of redness, dryness, thickening or lichenification
- Any signs of infection, crusting or pus
- Scratch marks, bleeding points or nodules from chronic rubbing
We may use clinical scoring systems to classify severity, which helps track progress over time.[4,5,8]
When tests like allergy panels, blood tests or biopsy are advised
In many cases, eczema diagnosis is clinical and no tests are needed. Tests may be suggested if:
- There is doubt between eczema and other skin diseases
- We suspect contact allergy and need patch testing
- There are frequent or severe infections, or poor response to standard care[4,5,7]
- We plan certain advanced treatments that require baseline blood work
We discuss every test with you so you understand why it is being done and how it may change management.
How eczema treatment works at our clinic
Step 1: Repairing the skin barrier
High quality emollients (moisturisers) are the foundation of eczema care. Guidelines recommend generous, regular use of moisturisers even when the skin looks clear.[1,4,5] We help you choose textures and formulations that suit Mumbai’s humidity and your daily routine.
We also advise on:
- Gentle, fragrance-free cleansers
- Short, lukewarm baths or showers
- Pat-drying with a soft towel and applying moisturiser within a few minutes
Step 2: Prescription topical medicines for flares
During flares, prescription creams or ointments may be needed to control inflammation. These can include topical steroids of appropriate strength or non-steroidal options such as calcineurin inhibitors.[1,2,4,5]
Your dermatologist will decide which product to use, which body area to apply it on and for how long, based on Indian and international guidelines and your skin’s response.
Step 3: Itch control and sleep support
Persistent itching can be very distressing. We focus on:
- Barrier repair and anti-inflammatory creams to address the root cause
- Simple measures like cool compresses and keeping nails short
- In selected cases, short-term medicines at night to help with itch and sleep as per guidelines[4,5]
Step 4: Managing triggers
We work with you to identify patterns and triggers such as:
- Heat, sweat, friction from clothing
- Strong soaps, detergents or sanitisers
- Certain fragrances, metals or hair dyes
- Ongoing stress and lack of sleep
Small, practical changes in daily routine often make a noticeable difference to flare frequency.[3,4,7]
Step 5: Advanced options
For moderate to severe eczema that does not respond adequately to topical treatment alone, guidelines support options like phototherapy (light-based treatment), systemic tablets or injectable therapies that act on the immune system.[1,2,6]
These are considered only after careful discussion of benefits, side-effects, monitoring and practical aspects such as visits and blood tests. They are usually reserved for selected patients where simpler measures are not enough.
Session plan and comfort: what to expect during visits
Your first eczema consultation in Mumbai
During your first visit at The Bombay Skin Clinic (Kemps Corner, Bandra, Andheri West or Chembur), we usually:
- Take a detailed history and examine your skin
- Review any previous medical records or products you bring
- Classify the severity and pattern of your eczema
- Share a written or digital plan with skincare, medicines and follow-up
You will have time to ask questions so you leave with clarity and realistic expectations.
Follow-up visit schedule during an active flare
For active flares, many patients need:
- More frequent follow-ups in the initial phase (for example, every 2–4 weeks) until the flare is controlled
- Adjustments to creams, moisturisers and trigger management based on response
The exact schedule is personalised. We also use photos and digital follow-up where appropriate to reduce travel when possible.
Maintenance visits once eczema is better controlled
After the skin becomes more stable, visits are spaced out. Maintenance visits focus on:
- Preventing new flares
- Fine-tuning daily skincare
- Addressing pigmentation marks and dryness
- Planning ahead for seasons or life events that often trigger flares
Comfort during treatment: pain, irritation and how we minimise it
Most eczema treatments are applied on the skin and are generally well tolerated. Occasionally, some people experience temporary stinging or warmth when starting certain creams. We minimise discomfort by:
- Repairing the skin barrier first with moisturisers
- Explaining the correct order and method of application
- Starting gradually on sensitive areas like the face, eyelids and neck when needed[2,4]
Downtime: can you work, travel and exercise during treatment?
Daily routine changes
Most people can continue their regular office work, studies and home duties while receiving eczema treatment. You may need to:
- Switch to softer, breathable fabrics such as cotton
- Carry a small moisturiser for re-application in air-conditioned environments
- Limit very hot showers and harsh soaps after long commutes
School and outdoor play in children with eczema
Children with eczema can usually attend school and play outdoors. Practical tips include:
- Applying moisturiser before school and after coming home
- Keeping nails short to reduce skin damage from scratching
- Informing teachers about the condition and any medicines, if needed
Travel, holidays and special events
Travel and special occasions are possible with advance planning. We help you create a simple travel kit with moisturiser, prescribed creams and basic instructions. This reduces anxiety and sudden flares when you are away from home.
Safety, side-effects and contraindications
Safe use of topical steroids and calcineurin inhibitors
Topical steroids and calcineurin inhibitors have an important role in eczema management when used correctly. International and Indian guidelines support their use with appropriate strength, duration and follow-up.[1–3]
We focus on:
- Choosing the right molecule and potency for each body site
- Using them for the shortest required period during flares
- Explaining fingertip unit methods and application frequency based on guidelines
- Reducing and stopping safely to avoid rebound problems[2,3,5]
When to be careful with oral medicines and injections
Oral or injectable treatments that act on the immune system need careful selection and monitoring. They are usually reserved for:
- Moderate to severe eczema not controlled with topical care
- Frequent flares that strongly impact quality of life[1,2,6,8]
Before starting, we discuss possible side-effects, tests required and follow-up schedule. We also check for any other health conditions or medicines that may interact.
Who should avoid certain treatments
Some medicines are avoided or used with extra caution in:
- Pregnant or breastfeeding women
- People with active infections (such as tuberculosis, viral infections, uncontrolled bacterial infections)
- Patients with significant liver, kidney or blood disorders
Your dermatologist will coordinate with your physician when needed so that your treatment remains as safe and balanced as possible.[1–4]
When to call your dermatologist or stop a medicine
You should contact us promptly if you notice:
- Sudden worsening of redness, pain or swelling after starting a medicine
- Extensive burning sensation that does not settle
- Unusual tiredness, fever or other systemic symptoms
Do not stop or change prescribed medicines on your own without advice, unless you suspect a serious reaction. In that case, seek urgent medical care and inform us as soon as possible.
Aftercare checklist for eczema-prone skin
Daily skincare routine
Many guidelines highlight that regular skincare is central to maintaining control of eczema.[1,3–5] In simple terms:
- Use a gentle, fragrance-free cleanser once or twice daily as advised
- Moisturise at least twice daily, and more often on very dry areas
- Use suitable sunscreen on exposed areas during the day
Bathing rules for Mumbai’s heat and humidity
In a hot and humid city like Mumbai:
- Prefer short showers over long hot baths
- Use lukewarm water, not very hot water
- Avoid scrubbing with loofahs or rough towels
- Apply moisturiser within a few minutes of gently drying the skin
Clothing, laundry and home environment tips
Simple adjustments like the following can reduce irritation:
- Choose soft, breathable clothes and nightwear
- Avoid tight, scratchy fabrics and labels
- Use mild, fragrance-free detergents and rinse clothes well
- Keep rooms well ventilated and not overly cold or dry from air conditioning
Diet, stress management and lifestyle support
Food triggers vary widely between individuals. Routine strict diets are not advised without clear evidence or medical guidance, especially in children.[3,4,6] Instead, we focus on:
- Watching for consistent patterns between certain foods and flares
- Maintaining a balanced, nutritious diet
- Helping you manage stress and sleep, as both influence flares
Simple at-home steps to manage a sudden flare
When a flare starts, helpful steps can include:
- Increasing moisturiser frequency
- Using prescribed anti-inflammatory creams as directed for flares
- Avoiding new cosmetic products or home remedies on active lesions
- Booking a quick review if the flare is not settling or if infection is suspected
What results to expect and realistic timelines
How soon do itching and redness usually improve?
With appropriate topical treatment and moisturising, many patients notice some relief in itching within a few days and clearer improvement in redness over one to two weeks.[1,5,6] The speed of response depends on severity, skin area and how regularly the plan is followed.
When do dark marks and dryness usually fade?
Dark marks (post-inflammatory pigmentation) and residual dryness often take longer to settle. It may take several weeks to a few months for the skin tone and texture to look more even. Patience and consistent skincare are important during this phase.
Long-term outlook: flares, remission and maintenance care
Eczema is generally a chronic relapsing condition. That means flares may come and go at different times of life. With good long-term care, many people enjoy long periods of clear or almost clear skin between flares.[1,3,6,8]
What treatment can and cannot do?
The aim of treatment is to:
- Reduce itching, redness and dryness
- Improve sleep, comfort and quality of life
- Decrease frequency and intensity of flares
Even with the best care, occasional flares may still happen. Our goal is to give you the tools, support and follow-up needed to manage these episodes early and confidently.
Eczema treatment options compared
Clinic-based eczema treatment vs home remedies
Home remedies such as random oils, herbal mixes or internet recipes may sometimes give short-term comfort but can also irritate the skin or delay proper care. Dermatologist-led treatment is guided by clinical evidence and safety data from large studies and guidelines.[1–4,7]
Prescription care vs over-the-counter creams and steroid mixes
Unsupervised use of over-the-counter steroid combinations, fairness creams or strong medicated creams can thin the skin, cause rebound redness or lead to other side-effects. In contrast, prescription care focuses on:
- Correct choice of medicine and strength
- Appropriate duration and tapering
- Safe long-term routines based on guidelines
Eczema treatment vs “skin allergy” treatments and fairness creams
Many so-called “skin allergy” treatments or fairness products contain hidden steroids or other strong agents. They are not the same as a structured eczema treatment plan, even if they temporarily reduce redness. Long-term, they can do more harm than good.
In-clinic care in Mumbai vs only online consultations / telemedicine
Online consultations can be useful in certain situations, but eczema often benefits from at least some in-clinic assessments where the dermatologist can examine the skin closely, assess texture and colour differences, and perform tests when needed. At The Bombay Skin Clinic, we combine in-clinic visits with digital follow-up where appropriate for convenience.
Special situations we often see in Mumbai
Eczema in babies and children
Childhood eczema is common in India and can cause significant distress to both the child and family.[3,6,8] We use age-appropriate products, explain routines to parents and align treatment with school and playtime needs. Growth, nutrition and psychological comfort are kept in mind.
Hand eczema in homemakers, healthcare and office workers
Frequent hand washing, cleaning, glove use or contact with chemicals can lead to stubborn hand eczema. We help you find a balance between hygiene and skin protection and, where relevant, consider patch testing for possible allergens.[3,7]
Eczema with asthma, allergic rhinitis and other allergies
Many patients have atopic conditions together, such as eczema plus asthma or allergic rhinitis.[3,6] In such cases, we may coordinate with allergists or physicians so that the overall allergy profile is managed in a unified way.
Eczema in people with busy travel and shift-work schedules
Mumbai has many professionals with irregular hours and frequent travel. For them, we design practical, minimal yet effective skincare and medicine plans that fit into their schedule and can be followed on the move.
Eczema treatment cost in Mumbai
What usually influences the cost?
The overall cost of eczema treatment in Mumbai depends on factors such as:
- Severity and extent of the condition
- Number of consultations needed to stabilise the skin
- Type and duration of prescribed medicines and moisturisers
- Need for tests like allergy panels or blood work
- Use of advanced treatments such as phototherapy or systemic therapies
Indicative pricing at The Bombay Skin Clinic?
At The Bombay Skin Clinic, an initial dermatologist consultation for eczema generally starts from around Rs.1,000 in Mumbai. Follow-up visits, medicines, moisturisers and any tests or procedures are charged separately. Exact costs depend on your personalised plan and will be clearly explained before you proceed. Fees are subject to change over time.
How we help you plan treatment within a realistic budget
We work with you to prioritise essential elements, such as effective moisturisers and prescription medicines, and avoid unnecessary products. Where possible, we suggest options at different price points and help you understand which parts of the plan are most important to maintain.
Why choose The Bombay Skin Clinic for eczema treatment in Mumbai?
Dermatologist-led, award-winning team
Our clinic is led by dermatologist Dr Batul Patel and a trained medical team with extensive experience in managing eczema and other chronic skin diseases. Treatment plans are based on recognised Indian and international guidelines and are adapted to each patient.
Multi-location convenience: Kemps Corner, Bandra, Andheri West and Chembur
The Bombay Skin Clinic has multiple locations across Mumbai, including Kemps Corner (South Mumbai), Bandra, Andheri West and Chembur. This makes it easier for you to access follow-up care close to home or work.
Advanced technology, gentle protocols and strict hygiene
We follow strict hygiene protocols, use evidence-based devices and therapies where indicated, and choose gentle yet effective skincare products suitable for Indian skin and Mumbai’s climate.
Personalised eczema care plans for adults and children
Every eczema plan is customised to age, lifestyle, occupation and family needs. We give special attention to children, working professionals, homemakers and elderly patients, as each group has different practical challenges.
Clear follow-up, digital reports and easy contact options
Our team stays in touch through reminders, digital records and easy contact channels. You can reach us via phone, WhatsApp or our online enquiry form to book or reschedule appointments and clarify basic doubts between visits.
How to prepare for your first eczema consultation with us
What to bring?
To make your first visit more effective, it helps to bring:
- Previous prescriptions, test reports or discharge summaries related to your skin
- Photos of earlier flares if your skin is currently better
- A list or photos of skincare, haircare and cosmetic products you are using
How to track symptoms and triggers before your visit?
If possible, note down for a week or two:
- When itching is worst (time of day, after which activities)
- Any clear relationship with soaps, weather, stress or specific foods
- Sleep patterns and how often you wake up due to itching
Even a simple note on your phone can give us valuable clues.
Questions you can ask your dermatologist
Feel free to ask about:
- Your exact diagnosis and severity
- Which creams and moisturisers are most important in your case
- How long you may need different parts of the plan
- What signs should prompt you to book an earlier review
A clear understanding makes it easier to follow the plan and manage flares calmly.
FAQs on eczema treatment in Mumbai
Is eczema contagious or can it “spread” to family members?
No. Eczema is not an infection and does not spread from one person to another through touch, sharing towels or living in the same house.[3,6] However, family members may share a tendency to develop eczema or other allergies because of common genes and environment.
Can eczema be completely cured or does it keep coming back?
Eczema is typically a chronic condition that tends to flare and settle at different times of life. Many people can achieve long periods of clear or almost clear skin with good long-term care, but occasional flares may still happen.[1,3,6,8] The focus is on long-term control, comfort and quality of life rather than promising that it will never come back.
Are steroid creams safe for long-term use on the face and body?
When used correctly under medical guidance, topical steroids are an important and generally safe part of eczema treatment.[1–3] Problems usually arise from using very strong steroids on sensitive areas, using them for too long without supervision, or applying over-the-counter mixed creams without knowing their contents. At our clinic, we follow guideline-based choices, explain how to apply them and monitor your skin closely.
What is the best moisturiser routine for eczema in Mumbai’s climate?
The best routine is the one you can follow consistently. In general, guidelines recommend generous, regular use of emollients, even when the skin looks clear.[1,3–5] In Mumbai, many patients do well with:
- A gentle cleanser and moisturiser twice daily
- Additional moisturiser on exposed or very dry areas during the day
- Texture (lotion, cream, ointment) chosen according to season, sweat level and your comfort
How do I manage my child’s itching and scratching at night?
Night-time itching is common and distressing. Helpful steps include:
- Applying moisturiser and prescribed creams as advised close to bedtime
- Using light cotton nightwear and appropriate room temperature
- Keeping nails short or using soft mittens for small children
- Following any night-time medicines or routines suggested by your dermatologist based on guidelines
If sleep is still very disturbed, a review visit is important so that the plan can be adjusted.[4,6,8]
When should I consider advanced options like phototherapy or biologic injections?
Advanced options are considered when:
- Eczema is moderate to severe and not adequately controlled with good topical care and moisturising
- Flares are frequent and strongly affecting work, school or emotional wellbeing
- There are medical reasons to limit certain topical or systemic medicines[1,2,6]
These decisions are made after a detailed in-clinic assessment, discussion of pros and cons, and evaluation of your overall health and lifestyle.
References and sources
- Chu DK, JTF Atopic Dermatitis Guideline Panel. Atopic dermatitis (eczema) guidelines: 2023 AAAAI/ACAAI Joint Task Force practice parameter. Ann Allergy Asthma Immunol. Available from: https://pubmed.ncbi.nlm.nih.gov/38108679/
- Davis DMR, et al. Guidelines of care for the management of atopic dermatitis with topical and systemic therapies. J Am Acad Dermatol. Available from: https://www.jaad.org/
- Rajagopalan M, et al. Guidelines on management of atopic dermatitis in India. Indian J Dermatol. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC6537677/
- National Institute for Health and Care Excellence (NICE). Atopic eczema in under 12s: diagnosis and management (CG57). Available from: https://www.nice.org.uk/guidance/cg57
- Frazier W, Bhardwaj N. Atopic dermatitis: diagnosis and treatment. Am Fam Physician. 2020;101(10):590–598. Available from: https://www.aafp.org/
- International Eczema Council. Global report on atopic dermatitis 2022. Available from: https://www.eczemacouncil.org/
- Jeskey J, et al. Atopic dermatitis: a review of diagnosis and treatment. J Pediatr Health Care. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC11627575/
- Mahajan R, et al. Evidence-based recommendations for managing atopic dermatitis in pediatric patients: IADVL Pediatric Dermatology SIG. Indian J Dermatol. Available from: https://pubmed.ncbi.nlm.nih.gov/40097336/

Dr. Batul Patel (Dermatologist)
Medical Director – The Bombay Skin Clinic
Dr. Batul Patel is an award winning certified dermatologist, honoured as the “Dermatologist of the Year 2023” at the national level by The Economic Times. View profile